Living with lupus can feel confusing and overwhelming, especially after receiving a diagnosis, but the right care can make a real difference. While there is no permanent cure, modern lupus treatments can effectively control symptoms, reduce flare-ups, and help protect vital organs. The goal of treatment for lupus is to manage inflammation, regulate the immune system, and improve overall quality of life.
In this blog, we’ll first explain what lupus is, its common symptoms, and how it is diagnosed, followed by a detailed guide on how lupus is treated and the treatment options available today to help people live well with the condition.
For ongoing lupus treatments, Swyftscripts delivers essential SLE medicines and specialty medications for lupus straight to your door, making consistent care simple and stress-free.
What Is Lupus
Lupus is a long-term autoimmune disease where the body’s immune system becomes confused and attacks healthy parts of the body instead of protecting it.
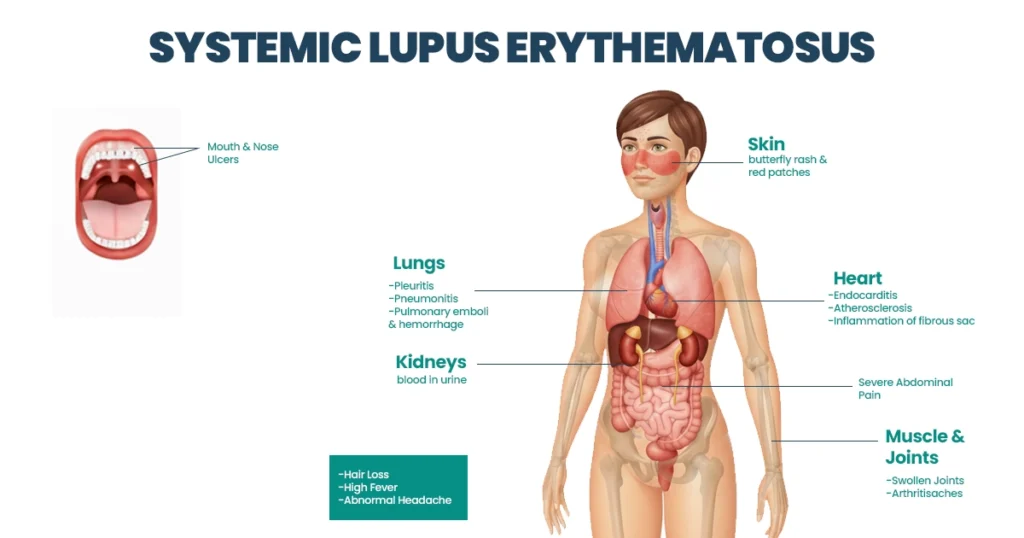
This can cause inflammation, pain, and damage in areas like the joints, skin, kidneys, heart, or other organs. Symptoms can come and go, and with proper medical care, many people with lupus can live normal, active lives.
The most common form of lupus is systemic lupus erythematosus (SLE). According to the CDC, more than 200,000 people in the United States are living with SLE, making it the most widespread type of lupus. Globally, an estimated 3.4 million people live with lupus, and about 90% of those affected are women, highlighting how disproportionately the condition impacts females.
Symptoms of Lupus Disease
Symptoms of lupus can vary widely from person to person and often fluctuate in cycles called flares. While anyone can develop lupus, women are affected more frequently and may experience certain symptoms more prominently.
Common symptoms of lupus:
Common symptoms of lupus include:
- Extreme fatigue, feeling unusually tired even after rest.
- Joint pain, stiffness, and swelling, often affecting the hands, wrists, and knees.
- Skin rashes, especially the characteristic butterfly-shaped rash across the cheeks and nose. Women may also notice rashes on other sun-exposed areas due to sensitivity to sunlight.
- Fever, unexplained and recurring.
- Hair thinning or hair loss, often diffuse, affecting the scalp.
- Mouth or nose sores, painless ulcers inside the mouth or nose.
- Chest pain or shortness of breath, caused by inflammation around the heart or lungs.
- Swelling in the legs, feet, or around the eyes, sometimes linked to kidney involvement.
- Headaches, memory problems, or difficulty concentrating, reflecting nervous system involvement.
- Cold or color-changing fingers and toes (Raynaud’s phenomenon), a circulation-related symptom more commonly noticed in women.
In women, symptoms like fatigue, joint pain, skin rashes, and hair thinning tend to be more prominent. Hormonal factors may influence flare-ups, especially during menstrual cycles or pregnancy.
Not everyone with lupus will have all these symptoms, and some people may only experience a few mild ones. Early recognition and proper treatment can help manage symptoms and prevent complications.
How Is Lupus Diagnosed?
Diagnosing lupus can be challenging because its symptoms often resemble those of other conditions and can vary widely from person to person.
According to the Lupus Foundation of America, many people live with symptoms for years before receiving a diagnosis. On average, it takes nearly six years from the first signs of lupus to a confirmed diagnosis. Because there is no single test that can definitively diagnose lupus, doctors rely on a combination of medical history, physical exams, laboratory tests, and imaging studies, often tracking symptoms and results over time.
Steps commonly involved in diagnosis include:
- Medical history and symptom review: The doctor will ask about your symptoms, their pattern, family history of autoimmune diseases, and any factors that trigger flare-ups.
- Physical examination: Checking for rashes, joint swelling, hair loss, mouth or nose sores, and other signs of inflammation.
- Laboratory tests: Blood and urine tests help detect abnormalities linked to lupus, such as:
- Antinuclear antibodies (ANA): Often present in people with lupus.
- Anti-dsDNA and anti-Smith antibodies: More specific markers for lupus.
- Complete blood count (CBC): To check red and white blood cells and platelets.
- Kidney and liver function tests: To assess organ involvement.
- Antinuclear antibodies (ANA): Often present in people with lupus.
- Urine tests: To detect protein or blood in urine, which may indicate kidney problems.
- Imaging tests: X-rays, echocardiograms, or other imaging may be used if lupus is suspected to affect the heart, lungs, or joints.
Because lupus can be unpredictable, doctors often diagnose it based on a combination of test results and symptom patterns over time, rather than a single definitive test. Early diagnosis and treatment are key to controlling symptoms and preventing serious complications.
Is Lupus Treatable?
Yes, lupus is treatable, but it is not curable.
Treatment focuses on managing symptoms, reducing flare-ups, and protecting organs rather than completely eliminating the disease. With the right combination of medications, lifestyle changes, and regular medical care, most people with lupus can lead active, fulfilling lives.
Key points:
- Medications such as NSAIDs, antimalarials, corticosteroids, immunosuppressives, and biologics help control inflammation and immune system activity.
- Lifestyle measures like regular exercise, a balanced diet, sun protection, stress management, and adequate rest support overall health and reduce flares.
- Early diagnosis and consistent treatment are essential for preventing serious complications and maintaining quality of life.
So, while lupus cannot be completely cured, it can be effectively managed with proper care.
Treatment for Lupus
While there is no cure for lupus, there are several effective lupus treatments available to help manage symptoms, reduce flare-ups, and protect vital organs. Treatment plans are personalized based on symptom severity, the type of lupus, and which organs are affected.
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
Nonsteroidal anti-inflammatory drugs (NSAIDs) are commonly used to reduce pain, swelling, and fever. They are especially helpful for managing joint and muscle discomfort, making daily activities easier for people living with lupus.
Antimalarial Drugs (e.g., hydroxychloroquine)
Antimalarial drugs, such as hydroxychloroquine, are frequently prescribed as part of lupus treatment options to control skin rashes, joint pain, and fatigue. These medications can also help prevent lupus flare-ups and protect organs from long-term damage.
Corticosteroids (e.g., prednisone)
Corticosteroids, like prednisone, are powerful anti-inflammatory SLE medicines used to control severe inflammation during lupus flares. While very effective, they must be used carefully, as long-term use can lead to side effects such as weight gain, bone thinning, or increased risk of infections.
Immunosuppressive Medications
For more severe cases, immunosuppressive medications may be prescribed to suppress the overactive immune system. These are particularly important for lupus that affects major organs like the kidneys or brain, helping to prevent serious complications.
Biologic Therapies (e.g., belimumab)
Biologic therapies, such as belimumab, target specific components of the immune system and are recommended as part of advanced lupus treatment options when other medications are not sufficient to control symptoms.
Lifestyle and Supportive Measures for Lupus
Managing lupus isn’t just about medications, lifestyle and supportive measures play a crucial role in controlling symptoms and improving overall well-being. Key strategies include:
- Regular exercise: Helps maintain joint flexibility, reduce fatigue, and improve mood.
- Balanced diet: Eating fruits, vegetables, lean proteins, and whole grains supports overall health and reduces inflammation.
- Sun protection: Wearing sunscreen, protective clothing, and avoiding direct sunlight can prevent skin rashes and flare-ups.
- Stress management: Techniques such as meditation, yoga, or mindfulness help reduce stress-related flares.
- Sufficient rest: Ensures the body recovers, helping to combat fatigue.
- Avoiding triggers: Being mindful of medications, infections, or extreme temperatures that can worsen lupus.
Combining these healthy lifestyle habits with prescribed lupus treatments can help people living with lupus manage their condition more effectively and maintain a better quality of life.
Get Your Lupus Medications Delivered with Swyftscripts
Managing lupus effectively requires staying consistent with your lupus treatments and SLE medicines. With Swyftscripts, you can have your essential treatment for lupus delivered safely and conveniently right to your doorstep. Avoid pharmacy lines, ensure you never miss a dose, and make it easier to stay on track with your health.
Visit Swyftscripts today and simplify your lupus care with reliable, stress-free medication delivery!