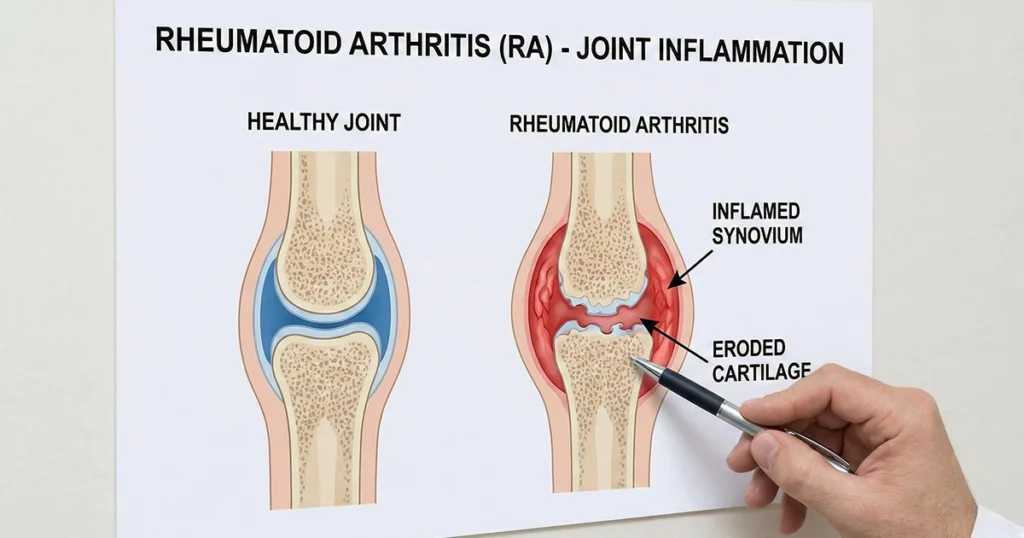
Imagine waking up every morning with stiff, swollen joints that make even simple tasks like gripping a coffee mug or tying your shoes feel exhausting. This is the daily reality for millions of people living with rheumatoid arthritis. Rheumatoid arthritis (RA) is a chronic autoimmune disease in which the immune system mistakenly attacks healthy joints, causing persistent inflammation, pain, and reduced mobility.
More than a joint condition, RA can affect the entire body, making early understanding and awareness essential for timely diagnosis and better long-term management. That’s where SwyftScripts comes in, a SCRIPT-certified service that manages your prescriptions from start to finish, handling insurance approvals, paperwork, and cost assistance, with free home delivery, so you can get your medications hassle-free and focus on your health.
What Is Rheumatoid Arthritis Disease
Rheumatoid arthritis (RA) is a chronic autoimmune disease in which the body’s immune system mistakenly attacks its own healthy joint tissue, particularly the lining of the joints (called the synovium). This immune‑driven inflammation leads to pain, swelling, stiffness, and can eventually damage the cartilage and bone in affected joints. It affects about 1 in 5 U.S. adults, highlighting how common joint conditions are in the population.
Over time, RA can also affect other parts of the body, including the lungs, heart, eyes, and blood vessels, and may cause joint deformities if not treated. It typically affects multiple joints on both sides of the body and is a long‑term condition that requires early diagnosis and ongoing management.
Is Rheumatoid Arthritis an Autoimmune Disease?
Yes, rheumatoid arthritis is an autoimmune disease. It occurs when the immune system, meant to protect the body from infections, mistakenly attacks healthy joint tissue. This abnormal immune response triggers chronic inflammation, leading to pain, swelling, stiffness, and progressive joint damage. Unlike osteoarthritis, which is caused by wear and tear, rheumatoid arthritis is driven by immune system dysfunction and can also affect organs beyond the joints, such as the lungs, heart, eyes, and blood vessels.
What Are the Early Signs and Symptoms of Rheumatoid Arthritis?
The early signs of rheumatoid arthritis often appear gradually and may be mistaken for normal aches or fatigue. Symptoms usually begin in smaller joints and tend to be persistent rather than occasional. Recognizing these early warning signs is important, as timely diagnosis and treatment can help slow disease progression and prevent joint damage. Below are some of the most common early symptoms to watch for:
- Morning stiffness lasting longer than 30–60 minutes
- Joint pain or tenderness, especially in the hands, wrists, and feet
- Swelling, warmth, or redness around affected joints
- Symptoms affecting the same joints on both sides of the body
- Fatigue, tiredness, or low energy levels
- Difficulty performing everyday tasks like gripping or walking
- Mild fever or a general feeling of being unwell
- Gradual worsening of symptoms over weeks or months
What Does Rheumatoid Arthritis Feel Like?
Rheumatoid arthritis often feels like persistent joint pain and stiffness that can make everyday movements difficult. Many people describe a deep, aching, or throbbing pain, especially in the morning or after long periods of rest, with stiffness that can last for an hour or more.
Joints may feel swollen, warm, and tender to the touch, and the discomfort usually affects both sides of the body equally, such as both hands or both knees. Beyond joint symptoms, rheumatoid arthritis can also cause fatigue, weakness, and a general feeling of being unwell, as the ongoing inflammation impacts the entire body.
What Are the 4 Stages of Rheumatoid Arthritis?
Rheumatoid arthritis progresses in stages, with symptoms and joint damage becoming more severe over time if left untreated. Understanding these four stages of RA can help patients and caregivers recognize changes early and seek appropriate treatment to manage pain and prevent long-term joint damage. Here’s a closer look at each stage:
- Stage 1: Early RA: In this initial phase, the immune system triggers inflammation in the joint lining (synovium), causing pain, stiffness, and swelling. X‑rays usually do not show any joint damage yet.
- Stage 2: Moderate RA: Inflammation begins to damage the cartilage that cushions joints. Symptoms like pain and reduced range of motion become more noticeable, and imaging may start to show early signs of joint changes.
- Stage 3: Severe RA: The disease progresses to where both cartilage and bone are affected. This leads to more intense pain, swelling, limited mobility, and often visible joint deformities.
- Stage 4: End‑Stage RA: This is the most advanced stage. The joints may be severely damaged or even fused, resulting in profound loss of function, ongoing pain, and very limited movement.
Not everyone moves through all four stages, especially with early diagnosis and effective treatment. Modern therapies often slow or halt progression and help preserve joint health.
What Causes Rheumatoid Arthritis?
Rheumatoid arthritis (RA) doesn’t have a single known cause; instead, it appears to develop when several influences combine to trigger abnormal immune activity. At its core, RA is an autoimmune disease, meaning the immune system mistakenly attacks the synovium (the lining of the joints), causing inflammation, pain, and joint damage.
The most widely supported factors involved include:
- Immune system malfunction: Something triggers the immune system to target healthy joint tissue, but researchers have not pinpointed exactly why this happens.
- Genetic susceptibility: Specific genes, especially variations in human leukocyte antigen (HLA) genes like HLA‑DRB1, increase the likelihood of developing RA, though having these genes doesn’t guarantee the disease.
- Environmental triggers: Smoking is one of the strongest risk factors linked to RA onset and severity. Other potential triggers include air pollution, occupational exposures (like silica dust), and certain infections.
- Hormonal and other factors: RA is more common in women than men, suggesting hormones play a role, and factors like obesity may also influence risk.
In summary, rheumatoid arthritis arises from a complex interplay between genetic predisposition and environmental or lifestyle factors, with the immune system ultimately misidentifying joint tissues as harmful and attacking them.
Is Rheumatoid Arthritis Genetic?
Yes, rheumatoid arthritis (RA) is influenced by genetics, but it isn’t strictly a directly inherited disease like some single‑gene disorders. Researchers believe that a combination of genetic and environmental factors affects whether someone develops RA. Certain variations in many genes, especially in the HLA‑DRB1 gene and other immune‑related genes, appear to increase susceptibility to the disease, and people with a first‑degree relative (such as a parent or sibling) with RA are at a higher risk than the general population.
However, having these genes doesn’t guarantee you’ll develop RA, and many people with RA have no family history of the condition. Environmental triggers like smoking, infections, or other factors also play a key role.
Who Is at Risk of Developing Rheumatoid Arthritis?
Here are the main factors that influence who is at risk of developing rheumatoid arthritis based on current medical research:
- Sex: Women are significantly more likely to develop RA than men, about two to three times as often.
- Age: Rheumatoid arthritis can develop at any age, but the risk increases with age. Most cases typically begin between ages 30 and 60, making middle adulthood the most common period for RA onset.
- Family history and genetics: Having a close relative with rheumatoid arthritis increases your risk. Certain genetic variations, especially in immune-system-related genes like HLA‑DRB1, are linked with higher susceptibility.
- Smoking: Long‑term cigarette smoking is a strong environmental risk factor and can also make RA more severe.
- Obesity: Being overweight is associated with a higher likelihood of developing RA.
- Gum disease (periodontitis): Severe gum infections have been linked to an elevated risk of RA.
- Other environmental factors: Exposure to air pollution and certain occupational dusts may contribute to RA risk.
How Is Rheumatoid Arthritis Diagnosed?
Diagnosing rheumatoid arthritis (RA) isn’t based on a single test; instead, doctors use a combination of medical history, physical examination, laboratory tests, and imaging to build a complete picture and rule out other conditions.
Here’s how RA is typically diagnosed:
- Medical history & physical exam: A healthcare provider will ask about your symptoms (such as when joint pain and stiffness started and how severe they are) and examine your joints for swelling, tenderness, warmth, or limited movement.
- Blood tests: Several blood tests help support an RA diagnosis by detecting inflammation and specific antibodies. Common tests include:
- Erythrocyte sedimentation rate (ESR) and C‑reactive protein (CRP) to assess inflammation levels.
- Rheumatoid factor (RF) and anti‑cyclic citrullinated peptide (anti‑CCP) antibodies are often present in people with RA.
- Erythrocyte sedimentation rate (ESR) and C‑reactive protein (CRP) to assess inflammation levels.
- Imaging tests: X‑rays, ultrasound, or MRI scans may be used to look for joint damage or inflammation that isn’t obvious on a physical exam. These help confirm RA and track progression over time.
- Specialist evaluation: A rheumatologist (a doctor who specializes in arthritis and autoimmune diseases) often makes the diagnosis using established criteria that combine symptoms, tests, and exam findings.
Because symptoms of RA can overlap with other conditions and not all tests are definitive on their own, the diagnosis is made by considering all the findings together rather than relying on any single test.
Simplify Your RA Treatment with SwyftScripts
Managing rheumatoid arthritis can feel overwhelming, from doctor visits to navigating medications and insurance. The key is timely treatment and hassle-free access to your prescriptions.
That’s where SwyftScripts comes in as a legit, SCRIPT-certified service that handles prescriptions end-to-end, including insurance approvals, complex paperwork, and cost assistance, so you receive your medications without stress. With free home delivery, SwyftScripts ensures your RA medications reach you safely and on time, letting you focus on living well.