Understanding how multiple sclerosis is diagnosed can feel overwhelming, especially when symptoms come and go or mimic other conditions. Many Americans experience years of uncertainty before finally getting answers, which is why knowing the steps, tests, and criteria involved is so empowering. This blog breaks everything down in a simple, supportive way so you can approach the process with confidence.
Multiple sclerosis (MS) affects everyone differently, and it’s estimated that over 1.8 million people worldwide live with the condition. Diagnosis rarely relies on a single test; instead, neurologists consider your symptoms, medical history, imaging results, and lab work to get a full picture. For patients managing MS, SwyftScripts simplifies access to specialty medications with cost-effective delivery and personalized pharmacy care. As you read through this guide, you’ll learn how experts rule out similar conditions, what happens during an MRI, and how brain lesions are evaluated to reach an accurate diagnosis.
When Is MS Usually Diagnosed?
Most people begin noticing symptoms in early adulthood, often between ages 20 and 40, when life is already busy with school, work, or family. Because the early signs can be subtle, like fatigue, numbness, or vision changes, many people delay seeking care. In 2021, MS was linked to nearly 4,740 deaths worldwide, highlighting its potential seriousness.
However, neurologists emphasize that early evaluation is crucial for slowing disease progression. The sooner multiple sclerosis is identified, the sooner treatment can protect nerve function and improve long-term outcomes.
What Age Is MS Diagnosed?
Although MS can technically appear at any age, diagnosis most commonly happens in young to middle-aged adults, with the average age of diagnosis being around 36 years. Pediatric and late-onset cases do exist, but they’re far less common. Doctors look closely at age-related patterns because they can help rule out other neurological conditions. And while age alone cannot confirm the disease, it does guide specialists toward the most appropriate testing and monitoring strategies.
Tests and Tools Used to Diagnose MS
Diagnosing multiple sclerosis requires a combination of advanced imaging, lab work, and neurological assessments. Because MS affects the central nervous system in different ways, doctors rely on several complementary tools to confirm inflammation and rule out similar conditions. Below are the core tests specialists use during the diagnosing process:
- Magnetic resonance imaging (MRI): MRI remains the most important tool for diagnosing MS. It detects inflammation, scarring, and brain lesions in multiple sclerosis, providing clear evidence of damage across the brain and spinal cord.
- Lumbar puncture: Often called a spinal tap, this test collects cerebrospinal fluid to check for oligoclonal bands, immune proteins commonly found in people with MS.
- Optical coherence tomography (OCT): OCT measures the thickness of the retinal nerve fiber layer, helping doctors identify optic nerve damage, which is common in multiple sclerosis.
- Evoked potential tests: These tests measure how quickly electrical signals move through the nervous system. Delayed responses can indicate nerve pathway damage caused by MS.
- Blood tests: While a multiple sclerosis blood test cannot confirm MS by itself, bloodwork helps exclude conditions that mimic MS symptoms, such as infections, autoimmune disorders, or vitamin deficiencies.
- Neuropsychological testing: This evaluation identifies cognitive changes related to memory, focus, processing speed, and problem-solving—functions that may be affected by MS.
- Neurologic exam testing: Neurologists assess reflexes, coordination, strength, sensation, and balance to identify patterns that align with MS-related nerve damage.
- Cerebrospinal fluid (CSF) analysis: This deeper analysis of spinal fluid helps confirm immune activity within the central nervous system, supporting MRI findings and clinical symptoms.
MRI for Multiple Sclerosis
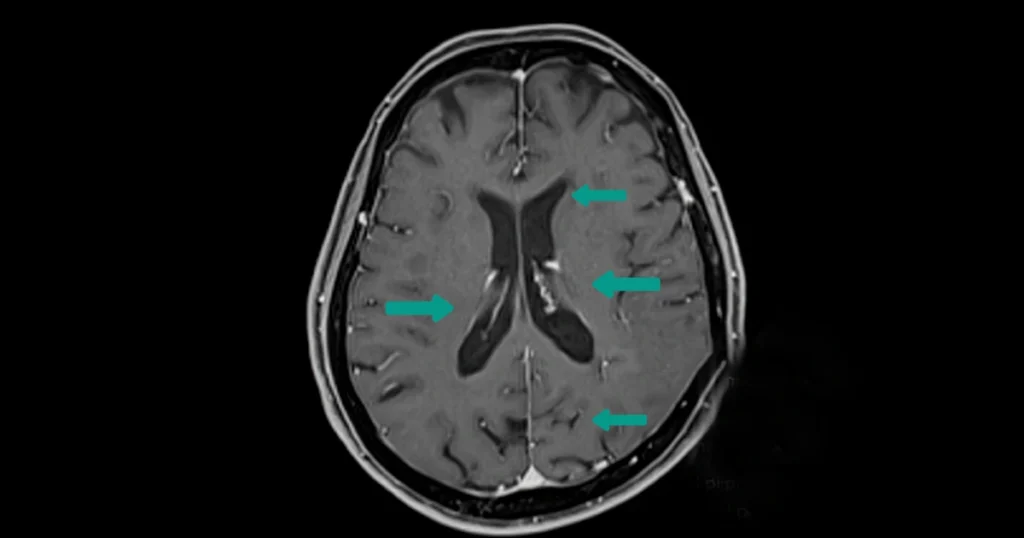
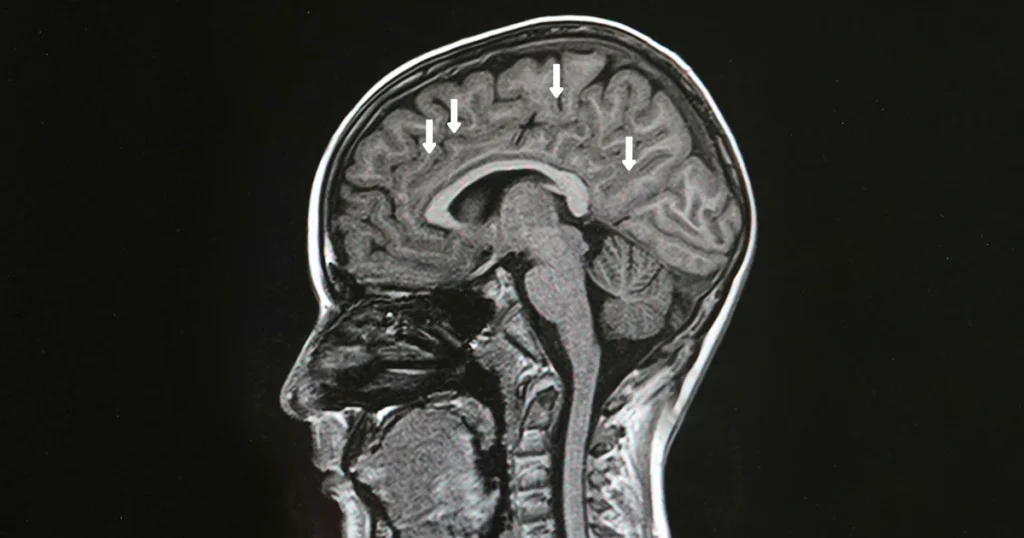
An MRI is one of the most important tools for diagnosing MS because it shows inflammation that isn’t always noticeable through physical exams. Neurologists pay close attention to brain lesions in multiple sclerosis, which often appear as bright spots on MRI scans. These lesions reflect areas where the immune system has damaged the protective coating around nerves.
MRI technology can also track disease progression over time, helping doctors tailor treatment plans. Follow-up imaging allows specialists to see whether new lesions have formed or existing ones have changed, which can guide decisions about medication adjustments or therapy updates.
Brain Lesions in Multiple Sclerosis
Brain lesions are a key marker of MS because they show areas where the immune system has damaged the myelin, the protective coating around nerve fibers. These lesions can appear in several regions, including the periventricular area, cerebellum, brainstem, and spinal cord. Their location often explains symptoms like numbness, poor coordination, or vision issues.
Understanding lesion activity helps neurologists determine how active the disease is. Over time, changes in lesion size or number can reveal whether treatments are slowing inflammation or if another medication may be necessary.
Multiple Sclerosis Blood Test: What It Can and Cannot Do
Although many patients ask for a multiple sclerosis blood test, there is currently no single blood test that directly diagnoses MS. Instead, bloodwork helps rule out conditions such as Lyme disease, lupus, vitamin B12 deficiency, and thyroid disorders. This step is essential because these issues can mimic MS symptoms, leading to confusion without proper testing.
Doctors may also use blood tests to check markers of inflammation or immune activity, supporting the broader diagnostic picture. While not diagnostic on its own, bloodwork ensures that the final diagnosis is accurate and not based on symptoms alone.
How Does MS Get Diagnosed?
MS is diagnosed using the McDonald Criteria, a globally recognized framework that evaluates lesions, location, and timing of symptoms. Neurologists look for evidence of “dissemination in space” (lesions in multiple areas of the CNS) and “dissemination in time” (lesions appearing at different stages). By combining clinical history with imaging results, they assess whether ongoing inflammation explains the patient’s experiences.
During this process, specialists may ask detailed questions about previous episodes of vision blurring, numbness, or balance issues. These conversations help determine whether undiagnosed flare-ups may have occurred in the past. Together, this information builds a timeline that supports or rules out multiple sclerosis.
Start Your MS Evaluation Today
Being evaluated for MS can feel intimidating, but understanding the diagnostic process makes it far less overwhelming. The combination of MRIs, neurological exams, and symptom history gives doctors the information they need to provide clarity and support. And once a diagnosis is confirmed, patients can begin exploring treatment options that protect nerve function and improve quality of life.
If you’re experiencing symptoms or have concerns, reach out to a neurologist as early as possible. Early diagnosis is one of the strongest tools for managing multiple sclerosis effectively. And if you need medications, at SwyftScripts, as a specialty pharmacy, we simplify access to treatments, offering cost-effective delivery and personalized care to support both patients and providers, making it easier to start and stay on your prescribed therapy.