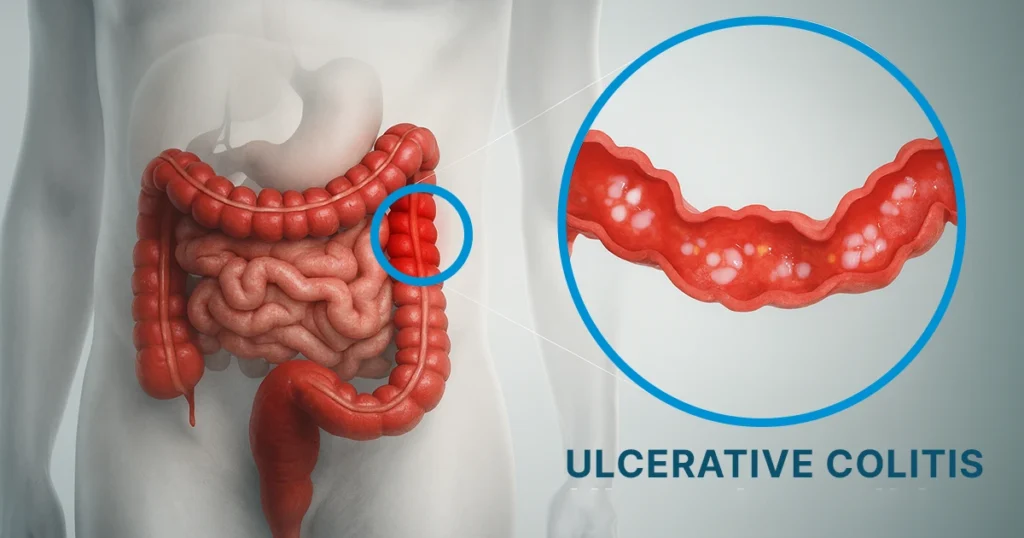
Treating ulcerative colitis starts with a combination of targeted medications, lifestyle adjustments, and timely medical care. Depending on the severity of symptoms, doctors may prescribe anti-inflammatory medicines, immunosuppressants, biologics, or small molecule therapies to control inflammation and prevent flare-ups. Alongside medical treatment, dietary modifications, stress management, and proper hydration play a key role in supporting remission and maintaining long-term colon health.
For patients managing ulcerative colitis, timely access to specialty medications can make a significant difference in controlling flare-ups and maintaining remission. SwyftScripts delivers specialty medications directly to your door, ensuring you receive the treatments prescribed by your gastroenterologist without delay. With reliable delivery, expert guidance, and support for medication management, SwyftScripts helps patients stay on track with their treatment plan, improving outcomes and supporting long-term colon health.
Ulcerative Colitis Treatment
Ulcerative colitis (UC) is a chronic inflammatory condition of the colon, with a prevalence exceeding 400 per 100 000 in North America. Managing UC effectively is essential because it affects thousands of people across the region, with symptoms ranging from mild discomfort to severe flare-ups that can disrupt daily life. Treatment typically starts with targeted medications and may include lifestyle adjustments or, in some cases, surgery to control inflammation and maintain remission.
Depending on symptom severity, doctors may prescribe anti-inflammatory medicines, immunosuppressants, biologics, or small molecule therapies. Combining these treatments with diet, stress management, and regular medical follow-ups helps many patients achieve long-term stability and improved quality of life.
Anti-Inflammatory Medicines
Anti-inflammatory medicines are often the first step for mild to moderate UC because they help calm inflammation in the colon lining. They work by reducing immune activity in the gut, which can quickly ease symptoms like diarrhea, bleeding, and abdominal pain. These treatments are usually well-tolerated but must be taken consistently to maintain remission.
Oral 5-aminosalicylates (5-ASAs)
5-ASAs can be prescribed for newly diagnosed patients as well as those experiencing mild flares. They help protect the colon lining, decrease inflammation, and support long-term maintenance. Brands vary, but the goal remains the same: reduce flare frequency and keep symptoms controlled.
Corticosteroids
Steroids are typically used short-term to manage moderate flare-ups that don’t respond to first-line medicines. They work quickly and effectively, but because of side effects, doctors gradually taper them off rather than keeping patients on long-term courses. The aim is fast relief with careful monitoring during use.
Immunosuppressants & Immunomodulators
These medications are recommended when UC becomes moderate to severe, or when patients depend too heavily on steroids. They help calm an overactive immune system and allow the colon time to heal. However, they require close medical supervision and regular blood work.
Azathioprine (Azasan, Imuran)
Azathioprine works by slowing immune responses that cause chronic inflammation. It’s often used to maintain remission, especially for patients who can’t tolerate other therapies. Since it affects immune activity, ongoing monitoring is essential to ensure safety and effectiveness.
Mercaptopurine (Purinethol, Purixan)
Mercaptopurine can be effective for long-term control and is sometimes paired with other medications for stronger results. Patients benefit from reduced flare frequency and improved remission stability. However, strict dosing, liver monitoring, and adherence to guidelines are important for safe use.
Biologic Medicines
Biologic medicines target specific immune pathways involved in ulcerative colitis, offering advanced treatment options for patients when standard medications aren’t enough. These therapies are usually prescribed for moderate to severe UC or when flare-ups become difficult to manage. In clinical trials, response rates for biologics and other advanced therapies are typically in the 30% to 60% range, highlighting their potential effectiveness while emphasizing the need for personalized treatment plans.
Biologics for ulcerative colitis are prescribed when symptoms persist despite standard treatments or when flare-ups become difficult to manage. Your gastroenterologist will determine which class fits your condition best, ensuring your treatment plan is tailored to your specific needs.
- Anti-TNF Agents: Anti-TNF agents work by blocking tumor necrosis factor (TNF), a protein responsible for inflammation in the gut. Medications like Infliximab (Remicade), Adalimumab (Humira), and Golimumab (Simponi) help calm inflammation, reduce diarrhea and bleeding, and maintain remission over time. These are often used when patients haven’t responded fully to anti-inflammatory or immunosuppressant medications.
- Integrin Receptor Antagonist: Vedolizumab (Entyvio) is an integrin receptor antagonist that works by preventing certain white blood cells from entering the gut lining. This gut-specific mechanism reduces inflammation effectively while minimizing systemic side effects, making it a great option for moderate to severe ulcerative colitis.
- IL-12/23 & IL-23 Inhibitors: For patients who do not respond to other therapies, IL-12/23 and IL-23 inhibitors can provide targeted relief. Medicines like Ustekinumab (Stelara), Mirikizumab (Omvoh), Risankizumab (Skyrizi), and Guselkumab (Tremfya) block specific inflammatory pathways in the immune system, helping to control chronic inflammation and improve overall symptom management.
Small Molecule Medicines
Small molecule medications work differently from biologics because they target inflammation from inside the cells rather than outside. They’re taken orally and can be effective for patients with moderate to severe UC.
- Tofacitinib (Xeljanz): This JAK inhibitor works by blocking signals that drive inflammation. It’s often used when patients don’t respond to biologics and requires regular monitoring.
- Upadacitinib (Rinvoq): Another advanced JAK inhibitor, Rinvoq provides rapid symptom improvement for many patients. However, because of potential side effects, it must be used under strict medical guidance.
These medicines can offer meaningful relief, but your doctor will balance their benefits with required monitoring and long-term safety considerations.
Ulcerative Colitis Surgery
While many patients manage UC successfully with medications, surgery becomes necessary when symptoms become severe, life-threatening, or resistant to treatment. It can also be recommended to reduce colon cancer risk or address complications like bleeding or toxic megacolon.
In some cases, ulcerative colitis surgery is the most effective option for restoring long-term quality of life. Although the decision can feel overwhelming, surgical outcomes are often excellent with the right preparation and recovery plan.
Proctocolectomy
A proctocolectomy removes the entire colon and rectum, eliminating the source of inflammation completely. Because UC only affects the large intestine, this surgery is considered the closest thing to a cure. Patients typically no longer experience UC symptoms afterward, although adjustments to digestion and lifestyle are part of recovery.
Ileoanal Anastomosis (J-Pouch) Surgery
During J-pouch surgery, surgeons create a small internal reservoir from the small intestine, allowing patients to pass stool normally without a permanent ostomy. This approach helps preserve bowel function and independence. Most patients experience major symptom relief, improved quality of life, and strong long-term outcomes after recovery.
Home Remedies for Ulcerative Colitis
Lifestyle changes play a powerful role in managing daily symptoms and supporting remission. While not a replacement for medical treatment, they can help reduce flare-ups and improve overall digestive comfort:
- Anti-inflammatory foods: Soft-cooked vegetables, oatmeal, white rice, lean proteins, and omega-3 rich options can help reduce gut inflammation.
- Avoid trigger foods: High-fat foods, spicy meals, caffeine, alcohol, and raw vegetables during flares may worsen symptoms.
- Low-residue diet during flare-ups: Reduces bowel movements and gives the colon time to rest.
- Hydration: Staying well-hydrated helps prevent dehydration from diarrhea.
- Stress management: Yoga, breathing exercises, journaling, or light meditation can calm the gut-brain connection.
- Sleep: Ensuring adequate rest supports overall gut health and reduces flare recurrence.
- Gentle exercise: Walking or low-impact stretching helps maintain digestive stability.
- Meal planning: Following a 7-day meal plan for ulcerative colitis can help structure meals to support digestion and prevent flare-ups.
Take Control of Ulcerative Colitis With the Right Treatment
Taking charge of ulcerative colitis begins with timely diagnosis, personalized treatment, and a proactive approach. Early intervention can reduce symptom severity, protect long-term colon health, and prevent complications. Working closely with your gastroenterologist ensures your plan evolves as your condition changes.
Managing long-term treatment is easier with SwyftScripts, which delivers specialty medications directly to your home. Licensed pharmacists provide personalized advice and support for medication adherence, helping patients maintain remission and improve overall colon health.